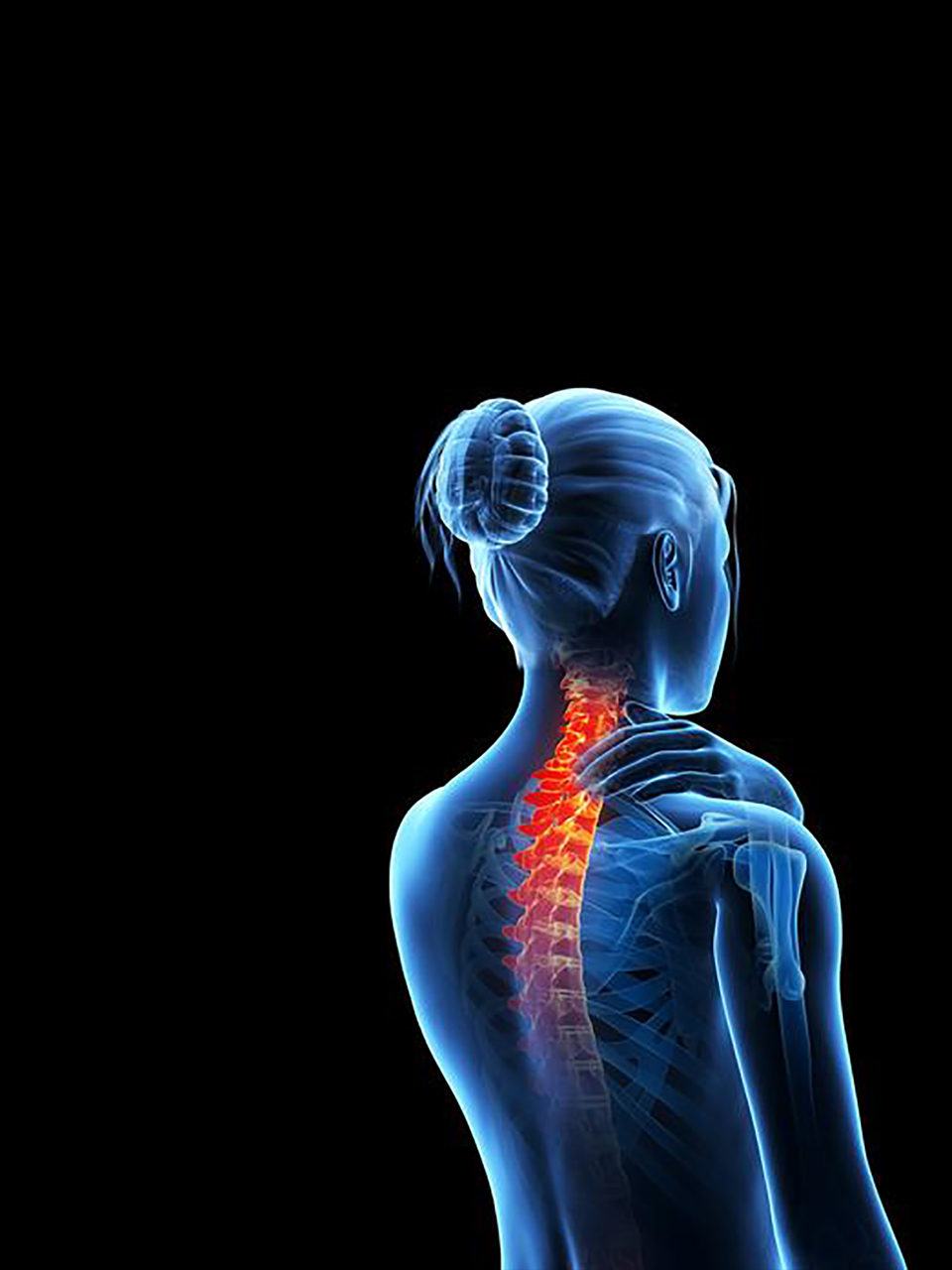
Osteoporosis, which means “porous bone,” is a disease in which the structure inside bones thins to the point where a slight fall or bump against a car door or piece of furniture can result in a fracture. A break can occur anywhere on your skeleton, although wrist, hip, and spine fractures are the most common.
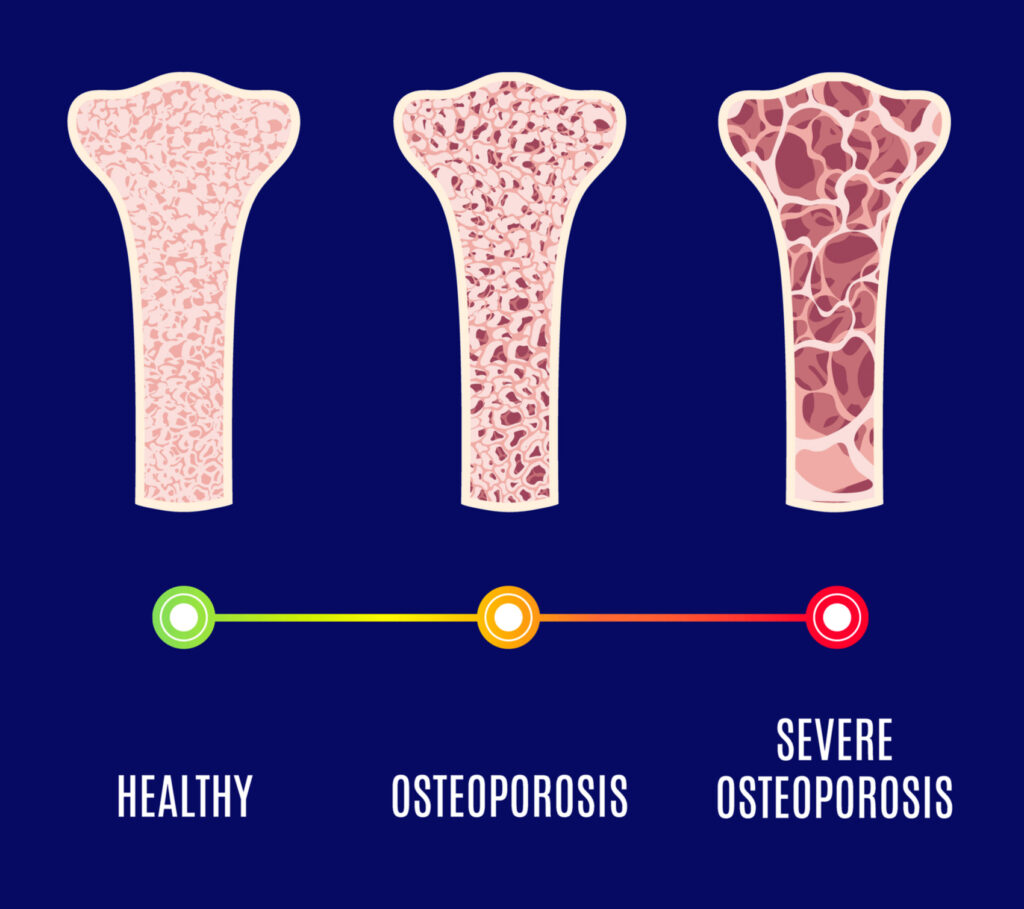
At any age, keeping your bones strong is a wise goal. A fracture-resistant frame becomes more important around 50 when weakening bones cause one in every two women and one in every five men to break. Fortunately, you can protect yourself from painful fractures at home and with the support of your doctor. Fractures can impair your independence and even raise your risk of dying from medical problems.
While age plays a role in osteoporosis, so do lifestyle practices and hormonal changes during childhood. Bone disease is caused by poor nutrition, lack of exercise, hormone shortages, and other harmful behaviours such as smoking and drinking. Bone loss begins in a woman’s mid-30s when estrogen and progesterone levels drop and accelerate in the first few years after menopause.
Because a person cannot feel their bones eroding, osteoporosis is a silent disease. However, because a fractured leg or hip can be painful and debilitating, the illness, in which bones become porous and brittle, is particularly serious in a woman’s elderly years. September is National Healthy Aging Month, so now is an excellent opportunity to check on your bone health.
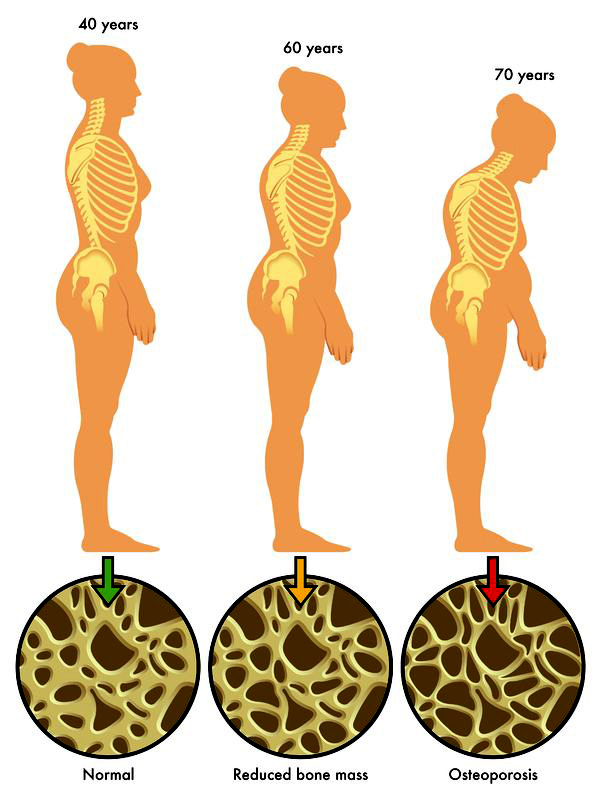
Osteoporosis symptoms
Osteoporosis has no signs or symptoms. So a bone density scan is the only way to find out what’s going on.
If you don’t have any substantial risk factors, such as smoking, taking big doses of steroid medicines, excessive drinking, or haven’t broken a bone in a non-traumatic event, she recommends getting tested at 65 for women and 70 for men. If you have any of these concerns, talk to your doctor about getting the test done at a younger age.
Fractures can occur spontaneously or due to minor falls or routine stressors such as bending, lifting, or coughing in osteoporosis-affected bones.
Risk factors for osteoporosis
Some risk variables, such as gender (women are at higher risk) and age, are unchangeable (as you get older, bone loss happens more quickly). Other options include:
Because they have less bone than larger-boned persons, slender, thin-boned people are more likely to develop osteoporosis.

White and Asian women are the most vulnerable. Women of colour and women of Mexican descent are at a lower risk. White men are more at risk than African-American and Mexican-American men.
If one of your parents has had osteoporosis or has fractured a hip, your risk of developing the condition is increased.
Endocrine and hormonal illnesses, gastrointestinal problems, rheumatoid arthritis, cancer, HIV, AIDS, and anorexia are all medical conditions that can raise your risk.
What can you do to lower your risk?
Calcium and vitamin D should be consumed as part of a healthy diet: If you do not consume sufficient calcium, your body will withdraw it from your bones, resulting in bone loss. Good sources of calcium include low-fat dairy products, dark green leafy vegetables such as spinach, bok choy, collards, turnip greens, sardines and salmon, broccoli, and calcium-fortified foods as soymilk, tofu, orange juice, and cereals.
Because all milk contains the same amount of calcium, low-fat or skims milk is the healthiest option.
When you reach age 45, have your primary care provider check your vitamin D level every so often to ensure it’s sufficient.
Exercise: “You want to do some resistance or weight-bearing exercises,” Climber said. “Walking is good for your bones. Using hand weights or bands to exercise or walking in a pool are good bone-building exercises. You don’t have to be in great physical shape to preserve bone, but you have to move.”
Do not smoke: Tobacco usage increases your rate of bone loss.
Limit alcohol: Too much alcohol can decrease bone formation. Women shouldn’t have more than one drink per day, and men no more than two drinks daily. Excessive drinking also increases the risk of falling.
Prevent falls: Remove electrical cords, area rugs and slippery surfaces in your home. Keep rooms brightly lit, install grab bars inside and outside the shower door, and make sure you can easily get into and out of bed.
What Can Women Do to Prevent Osteoporosis?
A woman can do or not do various things to build her bone structure and prevent osteoporosis. Women over 50 should consume 1,200 to 2,000 milligrams of calcium every day. One of the most effective strategies to prevent osteoporosis is to ensure that the body has plenty of calcium.
Calcium supplementation is especially necessary if you have any of the following conditions:
Vegan
A high-protein diet is recommended.
A high-sodium diet is recommended.
Have Crohn’s disease, IBS, or another health condition that prevents your body from absorbing calcium?
For an extended period, you’ve been on corticosteroids.
Fatty fish (salmon, tuna, sardines, mackerel, and trout), fish oils, egg yolks, and liver are all high in vitamin D. Another simple way to get vitamin
If you or someone you know has entered menopause, a bone density test should be taken to identify your risk of developing this condition. You can schedule an appointment with us to determine your osteoporosis risk. A Bone Mineral Density (BMD) test measures the density and thickness of the bones in the hip and spine using a pair of low-dose X-rays.
You won’t be able to see or feel your bones thinning or weakening. Health care practitioners employ bone mineral density (BMD) tests to diagnose osteoporosis. The BMD test assesses the number of minerals (calcium and phosphorus) in your bone to measure bone density. A low-dose X-ray called dual X-ray absorptiometry (DXA) of the hip and spine evaluates the density or thickness of your bones.
The T-score obtained from BMD testing compares your bone density to young, healthy persons of the same gender. A T-score of -1.0 or higher indicates normal bone mass. When your T-score is between –1.0 and –2.5, you may have low bone mass (osteopenia). When your T-score is –2.5 or lower, a BMD test will reveal that you have osteoporosis. While there is no cure for osteoporosis, this diagnosis will hopefully make people more aware of their risks and motivate them to do all possible to slow the disease’s progression.
Calcium is Important in Osteoporosis
You don’t have to be concerned about osteoporosis treatment. Make a strategy to boost your calcium consumption and make it a habit. Consult your doctor about the possibilities of hormone therapy for osteoporosis prevention. While it can help postmenopausal women avoid painful hip and spine fractures, it comes with its hazards. HRT users were shown to have an increased risk of blood clots, strokes, and breast cancer.
Whatever you do, please educate yourself on the disease to not be afraid of it. Also, keep clear of quicksand.