Dr. AmanyAyub MBBS, MPH
Public Health Specialist
In COVID 19 pandemic, availability and access to water, sanitation, and hygiene (WASH) services is fundamental to fighting the virus and preserving the health and well-being of millions. Universal, affordable, and sustainable access to WASH is a key public health issue within international development and is the focus of the first two targets of
Sustainable Development Goal 6 (SDG 6). Targets 6.1 and 6.2 aim at equitable and accessible water and sanitation for all. Unsafe care is often caused by poor infection prevention and control (IPC) practices, inadequate support for water, sanitation, and hygiene (WASH), and lack of adequate attention to waste management. A recent study on environmental conditions and standard precaution items in 129,557 health care facilities of 78 LMICs showed that only 2% of the facilities provided all four of water, sanitation, hygiene, and waste management services. Standard infection prevention and control (IPC) practices according to the national guideline, ensuring Water, Sanitation and Hygiene (WASH) component and adequate practices for environmental cleaning within the health care facilities has been considered as crucial for safe health care.
Additionally, availability of the Standard protocol and guidelines, link between IPC & WASH and trained health care providers on the various aspects of IPC, including the use of personal protective equipment, hand hygiene, proper use of antiseptics/disinfectants, and waste management are also extremely important part of quality improvement.
IPC and WASH also need to be addressed and integrated adequately into Quality of Care/Quality Improvement guidelines, tools, and processes.
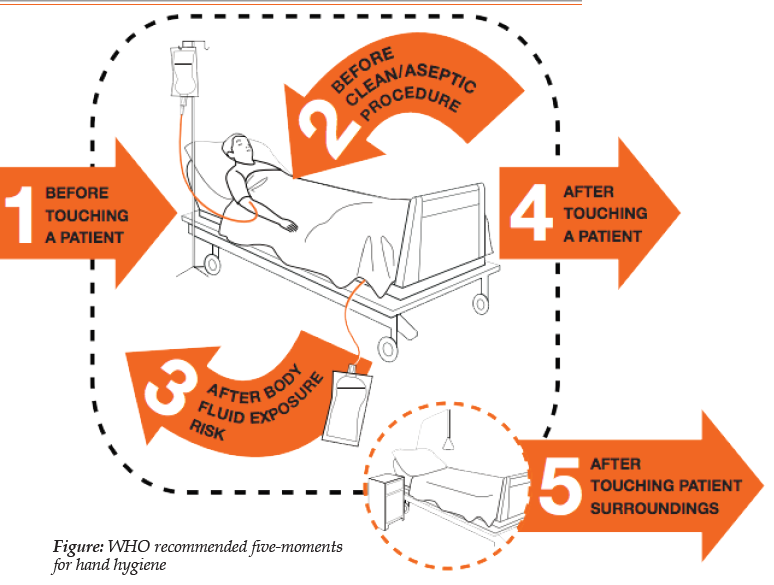
Hand hygiene
Any health-care worker, caregiver or person involved in direct or indirect patient care needs to be concerned about hand hygiene and should be able to perform it correctly and at the right time . Based on WHO-defined 5 critical moments, hand hygiene is required to reduce risk of pathogen transmission:
1. Immediately before touching a patient
2. Before clean/aseptic procedure (e.g. placing an indwelling device, opening venous access line, performing wound care)
3. After contact with body fluids or (secretions, excretions, and wounds) or contaminated surface
4. After touching a patient
5. After touching patient’s surrounding environment (items or surfaces known or likely to be contaminated)
1Cronk R, Bartram J. (2018). Environmental conditionsin healthcare facilities in low-and middle-incomecountries: Coverage and inequalities. International
Journal of Hygiene and Environmental Health 221(3): 409-422. doi:10.1016/ j.ijheh. 2018.01.004
2https://www.who.int/gpsc/5may/Hand_Hygiene_ Why_How_and_When_Brochure.pdf
Seven steps hand washing technique by WHO
1. Wet your hands with clean — preferably running — water.
2. Apply enough soap to cover all surfaces of your hands and wrists.
3. Lather and rub your hands together briskly and thoroughly. Make sure to scrub all surfaces of your hands, fingertips, fingernails, and wrists.
4. Scrub your hands and wrists for at least 20 seconds.
5. Rinse your hands and wrists under clean — preferably running — water.
6. Dry your hands and wrists with a clean towel or let them air-dry.
7. Use a towel to turn off the faucet.
The steps of hand rubbing are given below:
Step 1: Apply the alcohol-based hand sanitizer in a cupped hand (2 ml), covering all surfaces
Step 2: Rub hand palm to palm
Step 3: Right palm over left dorsum with interlaced fingers and vice versa
Step 4: Palm to palm with fingers interlaces
Step: 5 Backs of fingers to opposing palms with
Fingers Interlocked
Step 6: Rotational rubbing of left thumb clasped in right palm and vice versa
Step 7: Rotational rubbing, backward and forward with clasped fingers of right hand in left palm and vice versa
Step 8: Dry your hand in air
Environmental Hygiene
Two key principles of environmental hygiene are:
Step 1 – Cleaning:
• Clean BEFORE disinfection
• Clean with moping /washing with water-detergent
Step 2 – Disinfection
Disinfect items and surfaces that are:
• In contact with a patient’s secretion, touch or mucosa
• Frequently touched by healthcare workers
Type of disinfectants/decontaminants are:
• Soap, detergent,
• 0.5% sodium hypochlorite solution, (Chlotech, chlorox)
• Bleaching solution
• 70% ethanol
• Lysol
• Phenolic compound (e.g. Finish)
• 2% Glutaraldehyde ( Cidex )
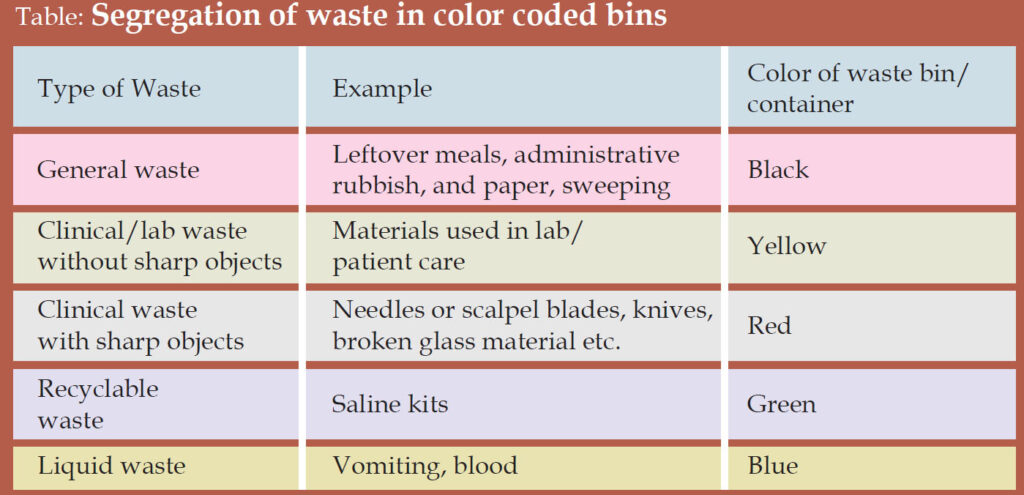
Waste Management
Waste management should be conducted in coordinationwith the infection control team.
There should be a person or persons responsible for the organization and management of waste collection, handling, storage and disposal. Waste management practices recommended as a general guide are:
• Keep waste in biohazard bag/waste bag in wastes bins
• Close/secure waste bag when two third to be filled up
• Record of generated wastes in designated temporary storage areas before disposal
• Treat the wastes by chemical decontamination
(0.5% sodium hypochlorite) or autoclave.
• Wash used linen (apron, hospital gown, sheets, and cotton blankets) in hot water (70°C to 80°C) with detergent and after that can soak in 0.1%Na-
OCL for 30 min then wash with water
• Manage wastes by incineration (ideal), if not available, do burning
• Burning waste in burial pits (>8 feet deep) in premises, behind the hospital building
• Set up a regular monitoring, reporting andappropriate capacity enhancement training planon infection control as well as management of waste disposal.
Implementing administrative controls
Hospital administration is responsible for ensuring IPC WASH practices in accordance with national guideline, relevant committees will supervise the IPC WASH activities. Hospital administration will designate a healthcare personnel to be the focal of IPC WASH activities of the healthcare setting. The responsibility includes:
• Establishing sustainable IPC infrastructures and activities.
• Ensuring adequate supplies of PPE, disinfectant, soap, hand sanitizer.
• Ensuring the adherence of IPC policies and procedures for all healthcare facilities.
• Ensure water.
• Improved sanitation facilities.
• Provision of adequate training for healthcare workers.
Reference
https://drive.google.com/file/d/1gURH__lKzI7Fz1zgzrV4Jg42UDzxE-1y/view

